Review of the latest literature shows life expectancy of people with HIV has dramatically increased since effective antiretroviral therapy has been available, and it continues to improve. Modelling studies suggest life expectancy could improve further with increased uptake of HIV testing, better antiretroviral regimens and treatment strategies, and the adoption of healthier lifestyles by those living with HIV. Early diagnosis is particularly important.
Harms of HIV infection
HIV treatments have radically improved quality of life and longevity for most people with HIV. This section provides a contemporary view of the physical consequences of HIV infection. It shows HIV can be effectively managed through medical treatment, health monitoring and healthy lifestyle, and that HIV-positive people taking treatment have a life expectancy similar to their HIV-negative peers.
Warning: file_put_contents(/home/hivjustice/apps/hivjusticetoolkit_live//wp-content/cache/headers_7aaae804fd24fd6d26382181fd0e4bcb_0.json): failed to open stream: No such file or directory in /home/hivjustice/apps/hivjusticetoolkit_live/wp-content/themes/hjntoolkit/functions.php on line 937
Warning: file_put_contents(/home/hivjustice/apps/hivjusticetoolkit_live//wp-content/cache/headers_78aab43c05a239a28ac8ecc154009f06_0.json): failed to open stream: No such file or directory in /home/hivjustice/apps/hivjusticetoolkit_live/wp-content/themes/hjntoolkit/functions.php on line 937
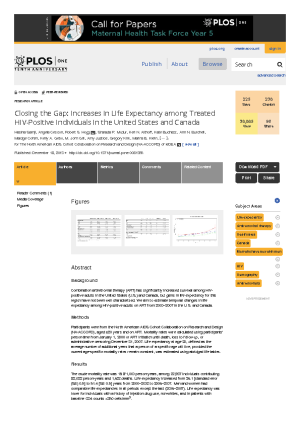
Closing the gap: increases in life expectancy among treated HIV-positive individuals in the United States and Canada
Estimates temporal changes in life expectancy among HIV-positive adults on ART from 2000–2007 in the U.S. and Canada. Found a 20-year-old HIV-positive adult on ART could expect to live into their early 70s, a life expectancy approaching that of the general population. Differences by sex, race, HIV transmission risk group, and CD4 count remained.
Warning: file_put_contents(/home/hivjustice/apps/hivjusticetoolkit_live//wp-content/cache/headers_0d2d85dad9993340eeb511883e9b3dcd_0.json): failed to open stream: No such file or directory in /home/hivjustice/apps/hivjusticetoolkit_live/wp-content/themes/hjntoolkit/functions.php on line 937
Mortality in well controlled HIV in the continuous antiretroviral therapy arms of the SMART and ESPRIT trials compared with the general population
Compares mortality rates in well controlled HIV-infected adults in two clinical trials with the general population. Found that HIV-infected individuals on ART with a recent undetectable viral load, who maintained or had recovery of CD4(+) cell counts to at least 500 cells/μl, had no increased risk of death compared with the general population.
Warning: file_put_contents(/home/hivjustice/apps/hivjusticetoolkit_live//wp-content/cache/headers_864fce2c71aa7aded95f464fdf16cb2f_0.json): failed to open stream: No such file or directory in /home/hivjustice/apps/hivjusticetoolkit_live/wp-content/themes/hjntoolkit/functions.php on line 937
Projected life expectancy of people with HIV according to timing of diagnosis
Estimates the life expectancy of an HIV-infected MSM living in a developed country with extensive access to ART and healthcare. Finds that predicted life expectancy is relatively high in people with HIV who can access a wide range of antiretrovirals. Finds the greatest risk of excess mortality is due to delays in HIV diagnosis.
Warning: file_put_contents(/home/hivjustice/apps/hivjusticetoolkit_live//wp-content/cache/headers_14b39724b7216734cbfc1a79dfd00b5e_0.json): failed to open stream: No such file or directory in /home/hivjustice/apps/hivjusticetoolkit_live/wp-content/themes/hjntoolkit/functions.php on line 937
Comparisons of causes of death and mortality rates among HIV-infected persons: analysis of the pre-, early, and late HAART (highly active antiretroviral therapy) eras
Finds that despite increasing concerns regarding antiretroviral resistance, the death rate among HIV-infected persons declined. A shift in the causes of death toward non-HIV-related causes suggests a more comprehensive health care approach may be needed for optimal life expectancy.
Warning: file_put_contents(/home/hivjustice/apps/hivjusticetoolkit_live//wp-content/cache/headers_14b39724b7216734cbfc1a79dfd00b5e_0.json): failed to open stream: No such file or directory in /home/hivjustice/apps/hivjusticetoolkit_live/wp-content/themes/hjntoolkit/functions.php on line 937
Risk of HIV Infection Per Single Sexual Exposure to an Individual Living with HIV, and Other Life Events Comparable Risk of Occurrence
Compares risk of HIV transmission from a single sexual encounter with odds of illness or death from other life events.
Warning: file_put_contents(/home/hivjustice/apps/hivjusticetoolkit_live//wp-content/cache/headers_9e64dc5cb4e23e8cb968d2efab7110fc_0.json): failed to open stream: No such file or directory in /home/hivjustice/apps/hivjusticetoolkit_live/wp-content/themes/hjntoolkit/functions.php on line 937
Criminalisation of HIV Non-Disclosure, Exposure and Transmission: Scientific, Medical, Legal and Human Rights Issues
This paper was commissioned by the UNAIDS Secretariat to serve as a background paper for the Expert Meeting on Criminalisation of HIV Non-Disclosure, Exposure and Transmission, 31 August – 2 September 2011, Geneva, Switzerland. It synthesises general considerations concerning issues raised by the application of the criminal law to non-disclosure, exposure or transmission in relation to HIV Scientific, Medical, Legal and Human Rights Issues.
Warning: file_put_contents(/home/hivjustice/apps/hivjusticetoolkit_live//wp-content/cache/headers_a3b216a88e2e59256f7e97fc551b1134_0.json): failed to open stream: No such file or directory in /home/hivjustice/apps/hivjusticetoolkit_live/wp-content/themes/hjntoolkit/functions.php on line 937
Bareback Sex in the Age of Preventative Medication: Rethinking the ‘Harms’ of HIV Transmission
This article provides a re-examination of the criminal issues relating to HIV transmission within the new landscape of advances in medical science and availability of PrEP and PEP, arguing that it necessitates a shift in attitude, policy and doctrine. It specifically argue that HIV transmission does not meet the appropriate harm threshold to constitute GBH and that if criminal law is ultimately about preventing or regulating harm, the ongoing criminalisation of HIV transmission is counter to that aim.